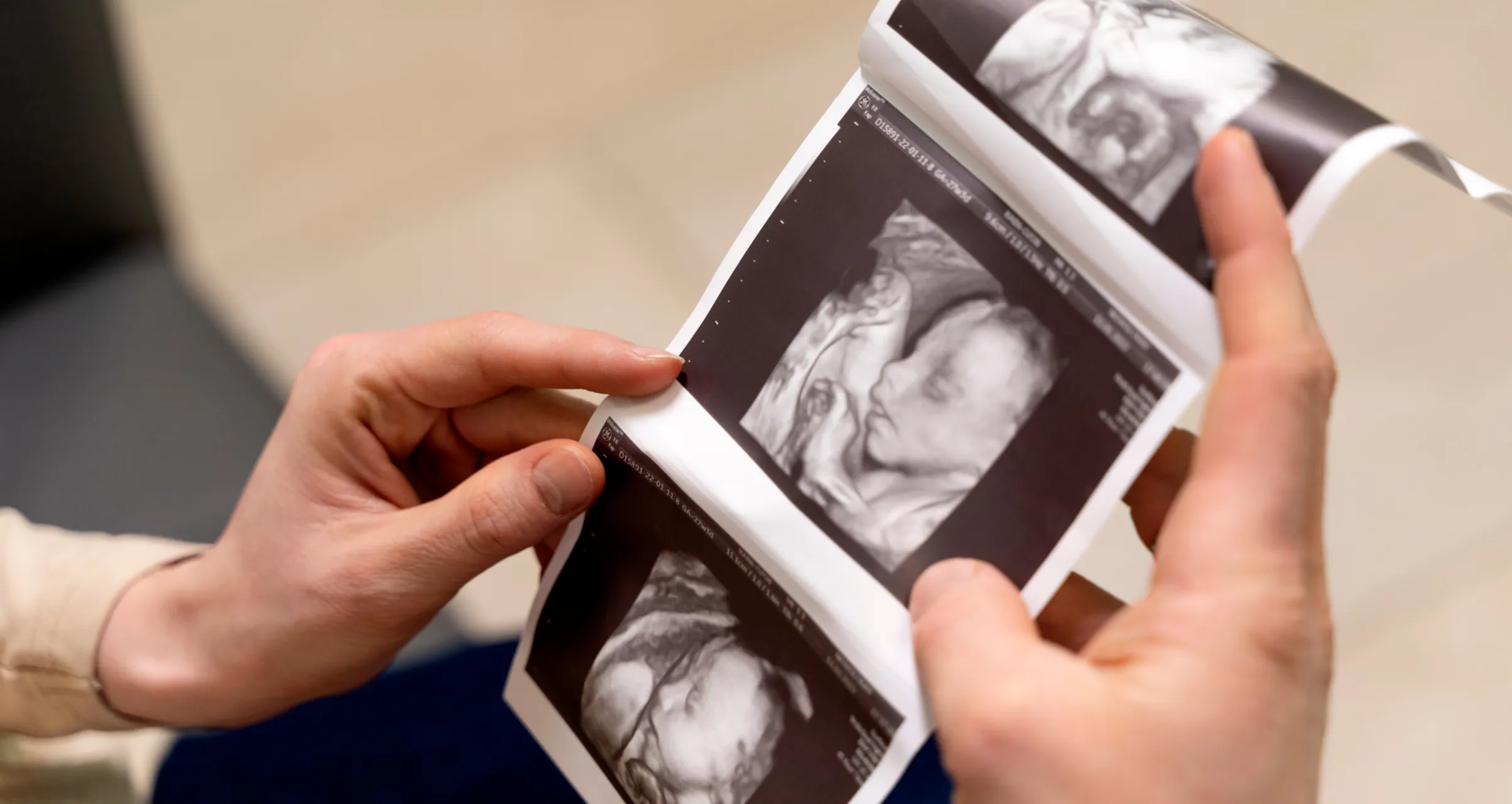
OBSTETRICS
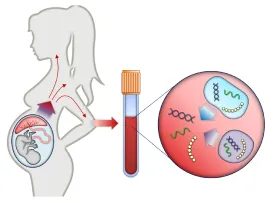
NIPT TEST
First Trimester Screening Is A Must To Rule Out Any Chromosomal Abnormality And Down Syndrome In Baby. With Simply Drawing Couple Of Ml Blood At 10 Weeks Gestation We Can Assure You About The Karyotype And Also We Can Find Out Gender Of Baby.
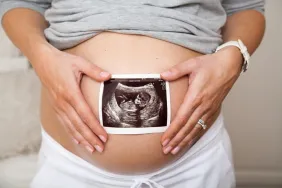
Pregnancy Ultrasound
Basically In First 12 Weeks We Use Vaginal Ultrasound And Later On Using Abdominal Ultrasound We Can Measure The Growth Of Fetus And Check Fetus Organs , Amniotic Fluid , Placenta Position And Fetal Presentation .
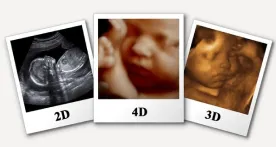
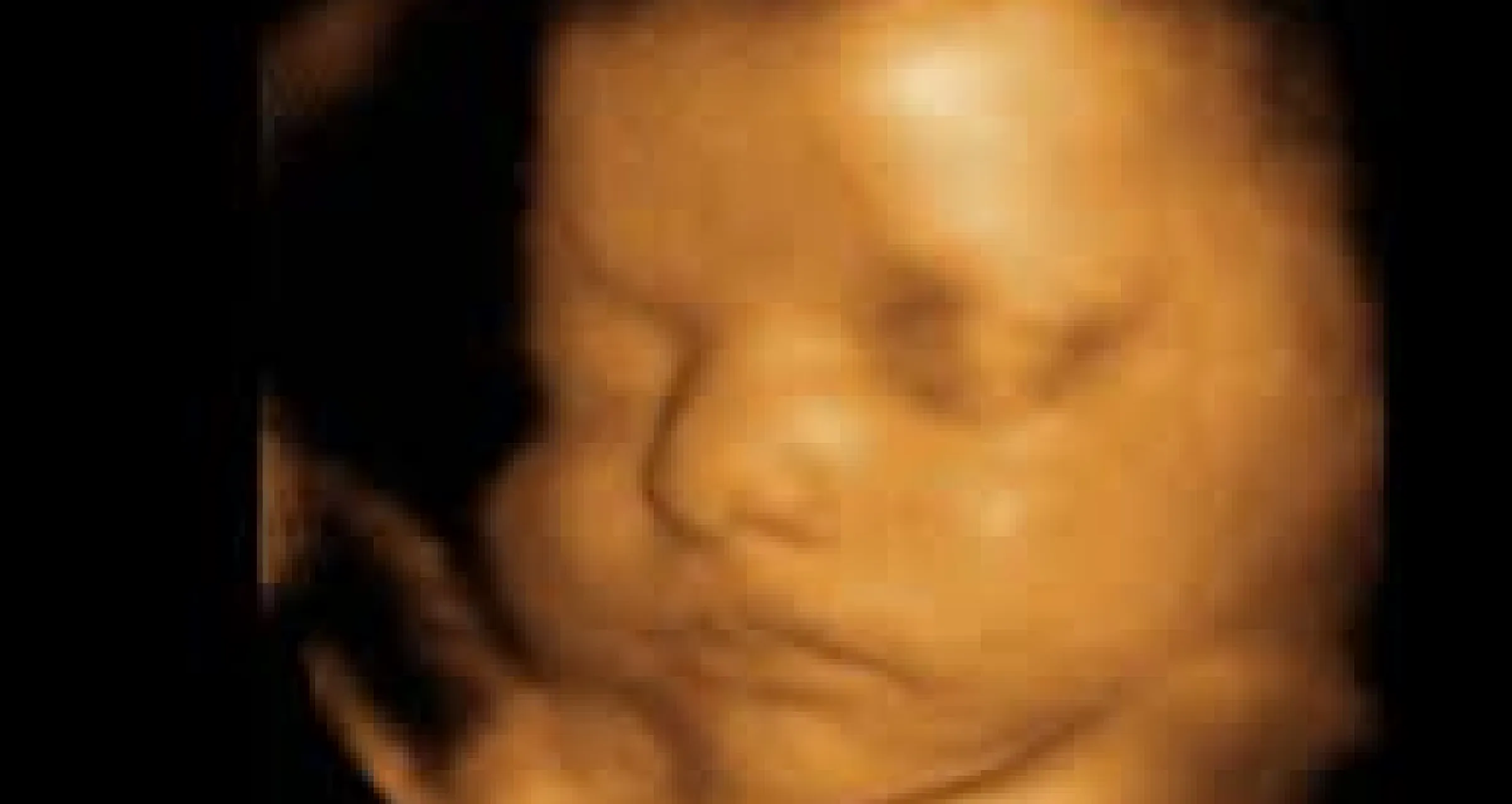
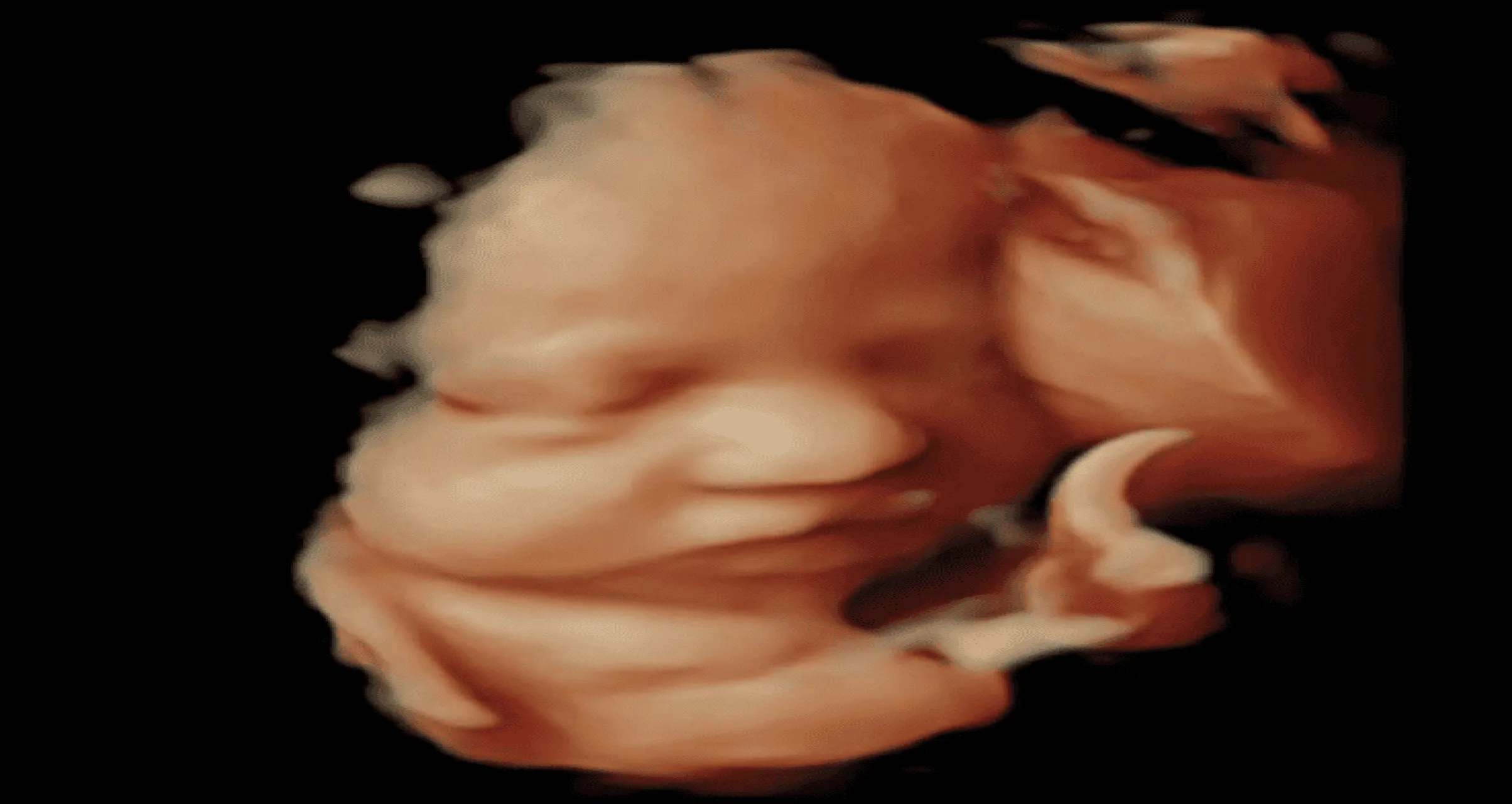
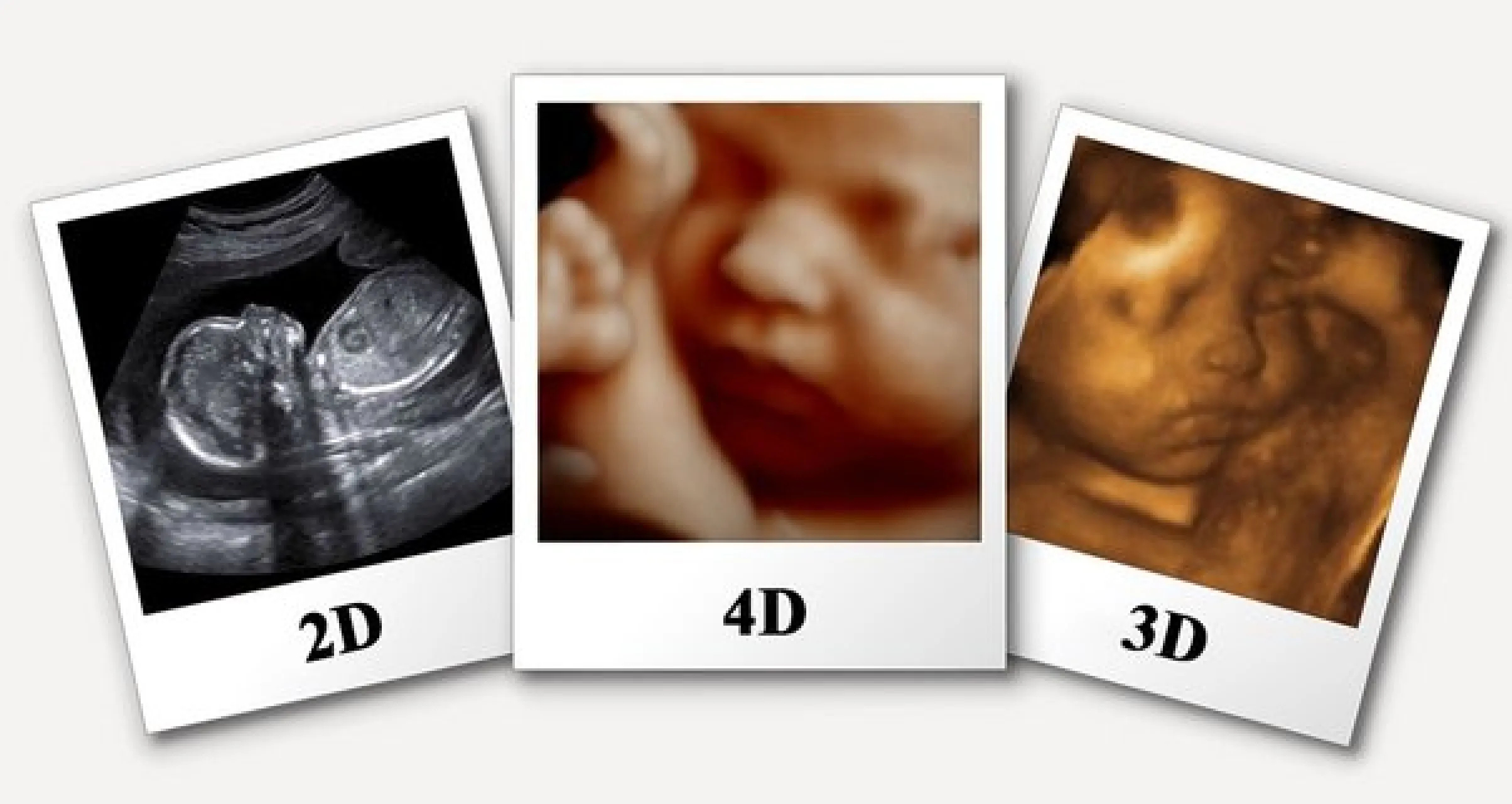
3D/ 4D Ultrasound
You Can Watch Your Baby Through 3D/ 4D Ultrasound Modality . Basically For Anomaly Scan We Use Regular 2 D Ultrasound And 3D/4D Is Only To What The Baby And See To Whom She Or He Looks Like ! Take Some Photos For Future Album And Get More Bounding With Your Baby Read More

Pregnancy Care Package
We Have Special Pregnancy Care Packages. For Normal Pregnancy Every 4 Weeks And For High Risk Pregnancy Every 2 Weeks . These Packages Starts From 12 Weeks And Covers Till Delivery
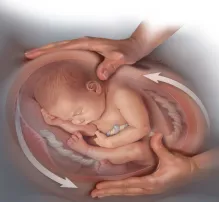
External Cephalic Version
In Breech Presentation , In Case It Meets Certain Criteria , Doctor Roya Does “External Cephalic Version ” To Change The Position Of The Head Of Baby From Breech To Cephalic To Avoid C Section Delivery . Currently Dr Roya Is The Only One In UAE Doing This Method ( Learn From Dr Zeinab Kazem Al Shunn

Normal Delivery C/ Section
We Are Affiliated With Emirates Hospital ( Jumeirah Branch ) . Dr Roya With More Than 20 Years Experience On NVD . VBAC( Vaginal Birth After C Section ) , Breech Delivery , Twins Delivery .Internal And External Cephalic Version